How to Optimize Recovery From ACL Surgery: Weeks 6-12
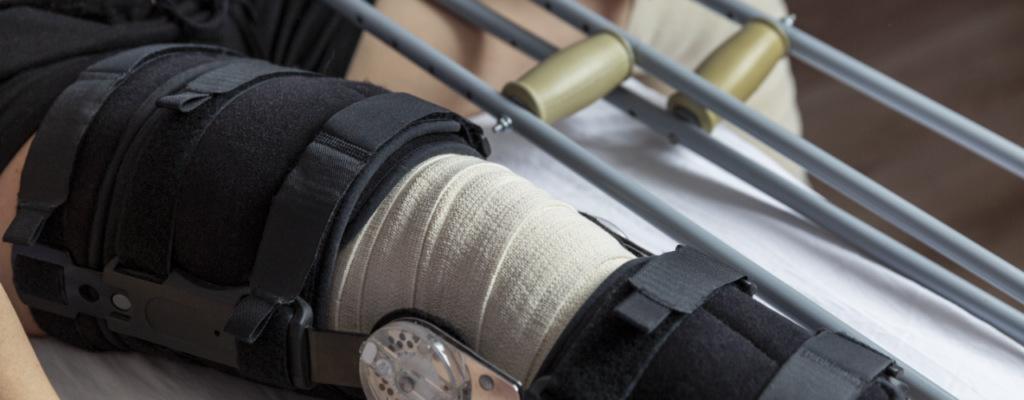
Welcome to phase 3 of your recovery from ACL surgery. This phase starts around 6 weeks after surgery and goes up until more or less 12 weeks post-surgery. While the time it takes to meet the criteria necessary to progress to phase 3 is malleable, the length of time required before moving to phase 4 really isn’t, which I’ll explain in a minute.
At this point you should feel pretty good. Your pain with normal activities like getting in and out of bed, walking, and standing up and sitting down should be minimal. It’s still common to have pain with higher-intensity activities, such as going up and down stairs and your rehab exercises. Your knee range of motion should also be close to full, and you should not have much swelling. Lastly, your knee should not feel like it’s giving out on you or unstable. If you’re still having problems with any of the areas I mentioned in the last 2 sentences, you’re not ready to move to phase 3 yet.
If you’re not to this stage of your rehab yet, you can check out my guides to phase 1 (0-2 weeks) and phase 2 (weeks 2-6) in the links. One thing to note: if you had surgery on your meniscus as well, there are additional precautions in addition to what I write about in this article, plus your rehab will probably be a little slower.
Your ACL Is Actually at Its WEAKEST Point Right Now
Your new ACL is 6 weeks old now, shouldn’t it be stronger than it was when you had surgery? The answer is actually no, and here’s why. During the first 4 weeks after surgery, part of the ACL graft dies off. This time frame is referred to as the “early graft healing phase” and is followed by a process of remodeling, during which the cells of the initial ACL that died off are replaced by new cells. Unfortunately, this process results in a significant decrease in strength of the graft until about the 6th week post-surgery, at which point the strength of the graft begins to increase again, with the greatest improvements noted until the 12th week post-surgery. At 12 weeks, the graft continues to undergo some continued improvements, but they are mild compared to what occurs in the first 12 weeks. This entire process is referred to a “re-ligamentization.”
I have attached a graph below that illustrates the relative strength of the ACL graft relative to the strength of an uninjured ACL. As you’ll see, the ACL graft is actually significantly stronger than the initial graft early after surgery, and if you were a superhuman and had no weakness, pain, or swelling after ACL surgery, this might be the time to set a new squat PR (please don’t try this). The graft then becomes progressively weaker, until it is actually weaker than the uninjured ACL, before slowly regaining strength until it is comparable to an intact ACL. From the research I have looked at, I would argue that the time points on the x-axis of this graph should be closer to 6 weeks and 12 weeks for the entire process, but there’s room for discussion. If nothing else, this graph is emphasizing that it would be unwise to try and return to sports before the 6-month mark. Overall, the re-ligamentization process takes several years, with the vast majority of changes occurring in the first 3-6 months.

If you have a decent physical therapist, they probably told you to NOT DO ANYTHING STUPID between weeks 7-12, and this is why. Your ACL is actually at its weakest point during this phase, which does not combine well with the inevitable urge of most people to start doing the things them love again because they’re finally feeling pretty good. While you might be able to get away with this, your risk of r-injury is very high, and you would be better served putting the effort you would put into your favorite activities into improving your strength, balance, and mechanics as much as possible.
Optimization Strategies
1. Maximize lower body strength and endurance
Like I mentioned in the last paragraph, this is the phase to really get after improving your overall strength, but especially lower body and core strength. During this phase, there are very few controlled exercises in the lower body that are off the table. This includes
- Squats/leg press
- Hamstring curls
- Calf raises
- Abdominal exercises
- Glute exercises
If you are performing these exercises with good control and good form, there is minimal risk of re-injury. In a minute, we will go through these exercises and discuss how to optimally use them, but first I want to discuss an idea known as periodization. In this context, periodization simply refers to changing the volume and intensity of an exercise on a regular basis to produce an intended effect. For example, if you perform an exercise one week at 80% of your 1-rep max (1RM) for 5 reps and progress to performing the same exercise the next week at 90% of your 1RM for 3 reps, that is an example of periodization. Following some sort of schedule similar to this will help to maximize improvements in strength while minimizing the risk of having your strength plateau.
Squats/leg press
My preference is to start with the leg press, since hip and ankle motion limitations are less likely to impact your ability to reach fatigue while maintaining good form during this exercise. Our primary goals during this phase are to maximize strength and muscle mass, and since you will have lost a lot of muscle mass in the quad by this point, it makes more sense to dose the exercise to improve muscle mass (aka hypertrophy), which will also lead to improvements in strength. Muscle mass is improved the most when sets are comprised of 6-12 reps, so I recommend starting with a weight that is challenging to perform for 12 reps. Perform 2-5 sets (the more the better, as long as you can adequately recover between sets and workouts) and shoot for twice per week. The next week, drop the reps to 10 and choose a weight that is challenging, which should be higher than the week before. This can be tricky, because ideally your strength will be coming back quickly, and most of the calculations we have for determining how much weight you should be able to lift for a given number of reps come from healthy individuals whose strength remains consistent across testing. You don’t have that luxury, so it’s ok to take a couple extra warm-up sets at a higher intensity to figure out what the best weight will be for you week-to-week.
Bonus: you can also use blood flow restriction when performing these exercises, which can yield similar results with less pain.
Hamstring curls
A concept we have not discussed before is the hamstring-to-quadriceps strength ratio, which refers to the maximum amount of force that can be produced with the hamstrings compared to the quadriceps. This ratio is important following ACL surgery, because the hamstrings are responsible for preventing anterior translation of the tibia (shin bone) on the femur (thigh bone), which is the primary motion that places stress on the ACL. By the end of your rehab, we want this ratio to be approximately 1:1, meaning that if you can produce 100 pounds of force with your quads, you can also produce 100 pounds of force with your hamstrings.
You have a couple different options to periodize your performance of hamstring curls for optimal results. While your quads will lose the most muscle mass after surgery, the hamstrings have likely lost a fair bit as well, so performing the same rep scheme I described for the squats/leg press is completely appropriate here as well. Alternatively, you can perform a rep scheme that is focused more on maximizing strength, rather than muscle mass, which means you would perform sets of 1-6 reps, instead of 6-12 (I know there’s overlap at 6). An example would be start with sets of 6 reps during the first week and move to sets of 5 reps, then 4, 3, etc.
Periodization also involves weeks of relative rest, which I am a fan of, even after surgery. I like to do 3-4 weeks of hard work followed by 1 easier week, where you still perform heavy lifting but with less volume. For example, if you are performing 3-4 sets of squats for 3 weeks with the rep scheme of 12 the 1st week, 10 the 2nd week, and 8 the 3rd week, then during the 4th week you would only perform 1-2 sets for 6 reps, but at a higher weight than you used the week before. Even though you are using a higher weight, the total volume is significantly lower, which allows your body to recover before starting another hard week.
Calves, abs, glutes, upper body, etc.
All the principles I described above apply to the rest of the muscle groups as well. Adding in ab routines, double- and single-leg calf raises (with weights when able), and upper body strengthening will help ensure you are not lacking in any department when it’s time to go back to your sport. If you don’t start working on these muscles now, it won’t get any easier down the road. Plus, working on full-body strengthening will help keep you in shape, since your relative energy expenditure during this phase is inevitably low compared to your baseline.
2. Optimize neuromuscular stabilization (NMS)
This is probably the most fun component of this phase because there are so many options and attention to detail really matters. This is where it’s important to work with a physical therapist or similar professional who is able to observe your movements from multiple angles and correct any poor movement patterns they might see.
Neuromuscular stabilization refers to the ability of your muscles and brain (via the nerves) to work together to perform desired movements. Every movement in life requires NMS, but I’m hoping you have mastered the easier ones like eating and walking so we can focus on movements that will translate to improved performance.
Balance
The first category of exercises that come to a therapist’s mind when you say NMS is balance, and for good reason. If you don’t have good balance, that makes pretty much every sport-specific movement harder to perform. Ideally, you have been working on basic balance exercises like tandem stance and single leg stance since the last phase, and you may have even started doing these exercises on unstable surfaces like a foam pad, Dyna disc, or bosu ball. If not, this is typically the phase to start incorporating these. This webpage gives a good rundown of a lot of different balance exercises you can begin incorporating. My favorite balance exercise, which also incorporates some strengthening, is to perform a single leg deadlift on a Bosu ball (flat side up) while holding a kettlebell in the arm opposite the leg on the ball. In addition to being good for balance and glute/hamstring strength, it will also test your ability to control your knee position while performing hip and trunk rotation.
Bonus: you can perform a lot of balance exercises on a whole-body vibration platform, which has been shown to significantly improve balance.
Single Leg Squat
NMS also refers to the ability to perform functional movements with good form. One of the movements that is typically agreed upon as being a good assessment of an individual’s overall ability to control their trunk and lower body movement during functional movement is the single leg squat; if you can’t perform this test well, it typically means you’re not ready to move on to phase 4. To perform this test, you stand on a 20 cm (8 in) box with one foot on, one foot off the side, perform a squat until your heel touches the ground (without putting pressure through that heel), and then return to the starting position. The goal is to be able to perform this movement without any bending or rotation in the trunk and no rotation in the hip or knee. When you’re first starting out with this exercise, you might need to use a walking stick or something similar in the hand opposite the leg on the box, which is completely fine.
Lunges
Another good exercise to begin performing during this phase is a lunge. The lunge is a great way to begin working on limb dissociation (i.e. one leg extended, the other leg flexed) and will give you a good estimate of your strength differences side-to-side. Surprisingly, most people find that performing a lunge with the surgical leg back is actually HARDER than performing a lunge with the surgical leg forward. You definitely need to do lunges on both sides to make sure you don’t have any deficiencies.
3. Cardio
Pretty much any type of cardio is fair game during this phase except for running – and possibly rowing, especially if you had work done on your meniscus during surgery. My favorites continue to be biking – especially biking on an assault bike because it’s a full body workout – as well as the elliptical and stair climber. If you like swimming, you can add that in as well.
You should also begin doing interval training during this phase. This can take many forms, for very high-intensity intervals like a Tabata set (I’ll explain in a minute) to longer-duration intervals. Below are a couple ideas of intervals that you can do.
- Tabata sets: 8 rounds of 20 seconds on, 10 seconds off. Can perform on a bike, stairmaster, rower, etc.
- 10 rounds of 30” on, 30” off
Time-Based Progression vs. Function-Based Progression
I am going to add a little aside here, because the end of this phase is when it starts to become important. While I have given benchmarks you should be able to meet to progress through the phases of ACL rehab, I have also given time frames. In many areas of surgical rehab, timeframes seem to have ultimate importance, such as not allowing weightbearing for a certain period of weeks after surgery or not returning to sports for a certain number of months. In most situations, these are primarily guidelines that are intended to be conservative and/or account for physiological healing times (as they are best understood at this point in time). However, it’s fairly obvious that there is a difference in the readiness to return to sports between an athlete that was consistent with their rehab program every day for 6 months and an athlete that trailed off after the first couple months when they started to feel good. Because of this, I highly recommend following a function-based progression, rather than a time-based progression when moving through the rehab stages. This becomes really important when moving from this phase to the next phase (phase 4), because that phase involves higher-intensity movements that could lead to re-injury.
This link will send you to the best function-based rehab progression I have found for ACL rehab. It more or less combines my first 3 phases into 2 phases, but their progression criteria for moving from this phase to the next phase are roughly the same. Their criteria include range of motion, swelling, balance, NMS control exercises, and a variety of strength exercises including single leg bridges, calf raises, core strength, and leg press. I highly recommend being able to complete each of the tasks they list in their phase 2 before moving on to running and agility drills.
Summary
Phase 3 of ACL rehab involves a lot more freedom in regard to the type of exercises you can perform. The primary goals of this phase are to optimize 1) strength gains in the injured leg, 2) balance and neuromuscular control with dynamic movements, and 3) cardiovascular endurance. You also need to remember that your ACL graft is at its weakest point during this phase, so this is not the time to try and show off your parkour skills. This phase is where you begin to build the base for performing all high-level activity. As always, I wish you the best with your rehab.
Western Slope Rehab and Performance is Here to Help
If you are struggling with injuries or have recently been in a motor vehicle accident, we can help. We are a physical therapy company that provides home-based orthopedic services in the Grand Junction, CO, area, as well as telehealth appointments throughout Colorado. If you would like to schedule a free consultation, you can call us as 970-462-9177, or fill out our contact form here.
If you found this post valuable, please like and share on our Facebook page, which is updated regularly with new content.

